Everyone experiences headache disorders differently. Some may have a sudden onset of debilitating migraine accompanied by a pulsating feeling behind their eyes, while others may have pain that feels like it originates from the base of the skull and extends to the neck and shoulders. This type of head pain is better known as a cervicogenic headache and it’s usually diagnosed and treated differently from other headaches.
So why do cervicogenic headaches happen and how do you cure them? Most cervicogenic headaches are caused by irritation, inflammation, or damage to the cervical spine structures. Treatment usually involves locating the source of the pain and administering appropriate procedures, such as occipital nerve blocks, trigger point injections, physical therapy, and chiropractic care, to address the specific spinal issue.
Cervicogenic Headache: Where and Why Does It Start?
Headaches are a common pain disorder that almost everyone can experience at any point in their life. This condition affects more than half of the global population, with at least 15% of the adult population in the United States experiencing its symptoms each year.
However, not all headache pain comes from the head or brain. According to studies, there’s one kind of secondary headache that accounts for at least 15% to 20% of reported headache complaints. This disorder is known as cervicogenic headache which is characterized by dull pain that runs from the neck to the scalp and spreads over the top or front of the head.
Cervicogenic headaches are a chronic disorder that mostly affects the adult population. Studies show that this head pain is prevalent among men and women who are 30 to 44 years old. Like most headache disorders, this condition can greatly affect your quality of life if left untreated for a long time.
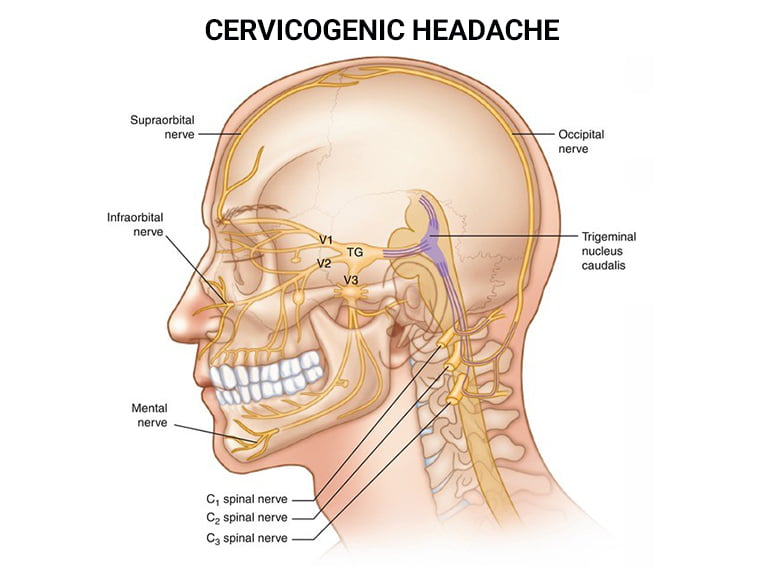
Understanding Your Cervical Spine
One thing you need to understand about cervicogenic head pain is that they’re completely different from your usual daily headache. As its name implies, it describes referred pain that originates from the nerves or structures in your upper cervical spine or neck.
To better understand how cervicogenic headaches occur, here’s an overview of your cervical spine and the different structures that may be involved in causing head and neck pain:
- Spinal cord and nerves – Your cervical spine is located at the topmost part of your spinal cord. It makes up the first seven vertebrae in the spine and starts below the skull and connects to the thoracic spine. There’s a total of 8 pairs of spinal nerves, labeled C1 to C8, in the cervical spine that are responsible for stimulating neck movement and sensation in your head and upper limbs. An inflammation or irritation to the specific C1, C2, and C3 nerves can cause flare-ups of neck and head pain.
- Neck muscles – Several muscles can also be found connected to your cervical spine. These include the deep cervical flexors, suboccipital muscles, trapezius, and levator scapulae which are all necessary for neck extension, head movement, or shoulder rotation. Any fracture, sprain, or trauma to these structures may develop cervical headache symptoms.
- Facet joint – These joints are found in between the bones of the spine. They help provide stability and facilitate different movements of the neck and head while also limiting the stress on the spinal structures whenever you twist or bend. If the joints become compressed or injured, it can cause cervicogenic headaches.
- Cervical discs – They serve as shock absorbers or cushions that prevent excessive force from damaging the vertebra. They also allow normal neck and head flexibility and support mobility. Any disc damage from traumatic injuries or natural degeneration due to aging can lead to pain in the neck and head.
6 Spinal Disorders That Can Cause Cervicogenic Headaches
When diagnosing cervicogenic headaches, doctors typically assess your spine health to determine if there are underlying problems that may be causing the chronic pain. Here are some of the possible spinal disorders that can lead to neck and head pain:
1) Whiplash Injury
This is a type of neck injury that occurs due to the rapid jerking movement of the neck muscles. You’ll likely acquire this after a car accident or due to incurring a strong blow to the head from a heavy object. The sudden motion causes the soft tissue and ligament of the neck to stretch and tear which can lead to excruciating headaches accompanied by neck stiffness, shoulder pain, and limited range of motion.
2) Slipped Discs
This condition happens when one of the discs in your vertebra becomes torn or damaged and slips out from its position in your spine. A slipped disc can happen after twisting or moving a heavy object which puts extreme stress on your cervical spine. Doing any physically demanding job or sports activity may also increase your risk for developing slipped discs.
3) Disc Degeneration
Neck pain and headache may also stem from cervical disc degeneration. This pertains to the natural wear and tear that occurs as you get older. With cervical degenerative disc disease, the discs lose their strength and structure which makes them unable to support your spine and leads to pain that can be felt at the neck, lower back, shoulders, and sometimes the head.
4) Pinched Nerves
Your headache may also be caused by cervical radiculopathy or pinched nerves in the upper cervical spine. This mostly happens due to compression or inflammation of a cervical nerve that results from a herniated disc or degenerative changes in your spine. When one of the nerves in your neck is affected, it can also cause pain in your arms, shoulders, and head.
5) Cervical Bone Spurs
Some cases of cervicogenic headaches also develop from having unusual growths on the bones of your cervical spine. This condition is also known as cervical osteophytes. Although most bone spurs don’t show symptoms, they can cause pain when it starts to compress the nerve endings in your cervical spine.
6) Osteoarthritis of the Cervical Spine
This condition refers to the natural changes in the joints, bones, discs, and ligaments of the cervical spine due to aging. Also known as cervical spondylosis, this spinal disorder can happen due to the breakdown of the discs and loss of flexibility of the joints that come with old age. Aside from headaches, this can also cause neck stiffness, weakness, and reduced range of motion.
Other Possible Triggers of Cervicogenic Headaches
The cervical spine naturally degenerates with age and becomes more prone to fractures and sprains, which is why older adults are more likely to experience chronic cervicogenic headaches. However, there are also other risk factors that may trigger neck and head pain among the younger population. Here are other common triggers of cervicogenic headaches:
1) Poor Posture
One of the leading causes of neck muscle strain is bad posture which can irritate the nerves in your cervical spine and compromise your spinal alignment. If you’re prone to doing excessive forward head position or protruding chin posture, you’re more likely to experience daily neck pain and headaches. That’s why you should constantly be mindful of your posture whenever you’re working in front of a computer.
2) Awkward Sleeping Position
Observing proper posture whenever you’re sleeping is as important as avoiding slouching during the day. Uncomfortable or awkward sleeping positions can develop neck pain, soreness, and stiffness in the morning.
One example is falling asleep on the couch without proper cushioning or support to your neck and head. This can lead to compressed spinal nerves which can worsen headaches and neck pain as soon as you wake up. Sleeping with your head drifting to one side or positioned too far in the front can also cause neck pain and stiffness.
3) Occupational Hazards
Cervicogenic headaches can also be a risk that comes with your profession. Some occupations that are likely to experience neck and head pain are hair stylists, drivers, construction workers, carpenters, and plumbers because of their working posture. Athletes who are exposed to strenuous activities and heavy lifting can also experience cervicogenic pain.
How to Tell If You Have a Cervical Headache
Some CGH symptoms may also be associated with another headache disorder. However, it can also cause other symptoms that can affect your vision, mobility, and sensation.
Here are other ways to know that you have cervicogenic headaches:
- Pain that spreads from the neck to one side of the head
- Pain that worsens whenever you try to move or rotate your neck
- Radiating pain at the scalp, forehead, behind the eyes, and temples
- Intense shoulder and arm pain
- Blurred vision
- Increased sensitivity to light and sound
- Nausea
- Vomiting
- Dizziness
Cervicogenic Headache vs. Other Headache Disorders: What’s the Difference?
Some of the symptoms of cervicogenic head pain may also be associated with another headache disorder. It’s important to know what type of headache you have to determine how you’ll treat your condition.
Here’s a table comparing cervicogenic pain from other kinds of headaches:
| Cervicogenic headache | Migraine headache | Tension headache | Cluster headache | |
| Main signs and symptoms | Pain at the head and neck and sometimes extending to the arms and between the shoulders Neck stiffness Reduced neck motion and flexibility | Severe headache or throbbing pain on one side of the head Nausea and vomiting Visual disturbances Increased sensitivity to light Can be acute or recurrent | Dull, aching pain across the head Feeling of tightness or intense pressure on one or both sides of the head | Intense headache with eye pain Sensitivity to light Swollen or drooping eyes Restlessness Eye redness |
| Causes | Originates from a problem in the cervical spine | Its exact cause is unclear but doctors suggest that it has to do with chemical activity that affects your blood vessels in the brain Can be triggered by hormone changes, stress, loud sounds, and bright lights | Usually occurs when the neck or head muscles contract or become too tense | It’s also unclear why cluster headaches happen but it’s thought to originate from the activity in the hypothalamus and trigeminal nerve |
| Outlook | Mild cases of cervicogenic headaches may resolve on its own, but some may require appropriate treatment that address the spinal problem | Can be easily managed with headache medications | A tension type headache can last for several minutes and go away on their own Painkillers can help provide relief from sudden tension headaches | They can go away on its own or with help of medications but may recur anytime without warning |
Treatment Options at Advanced Headache Center for Your Cervicogenic Pain
When your cervicogenic headaches start to disrupt your life and become accompanied by weakness and limited range of motion, you may need to visit a specialist for your condition. Most treatments for this type of head pain are meant to address the root of your pain: the cervical spine.
Here are some of the common ways that our doctors at Advanced Headache Center can treat your cervicogenic pain:
- Medications: Similar to treating migraines, cluster, and tension headaches, cervicogenic pain can also be improved by prescription drugs and over-the-counter painkillers. Some of the common medications for cervicogenic headache relief are analgesics, muscle relaxants, NSAIDs, and tricyclic antidepressants.
- Physical Therapy: You can also get neck and pain relief from physical therapy. This usually involves manual therapy and stretching exercises to reduce the pain and tension around your upper neck and shoulders. This can also help address your poor posture to lessen the recurrence of cervicogenic headaches.
- Chiropractic Care: Doctors also recommend chiropractic treatment to relieve pressure, inflammation, and tension on the affected joints, ligaments, soft tissues, and nerves in your cervical spine. One common example is spinal manipulation which helps improve the mobility and function of your cervical spine structures.
- Trigger Point Injection: This involves injections of an anesthetic mixture to certain pressure points in your neck and head which causes a chronic headache. For long-lasting relief, you can expect to receive multiple injections to address your pain.
- Occipital Nerve Block: This is a type of injection that’s placed at the back of the head and the neck to help minimize the inflammation and pain in the occipital nerves. It’s primarily given to address moderate to severe occipital neuralgia, as well as provide relief and comfort from cervicogenic headaches.
Get Relief from Cervicogenic Headaches at Advanced Headache Center
Cervicogenic headaches require more than just home remedies and painkillers. Doctors will need to examine your cervical spine health to rule out other conditions and recommend the best treatment for headache and neck pain relief.
At Advanced Headache Center, our doctors have extensive experience in diagnosing and treating different kinds of head pain. We can provide a comprehensive treatment plan that involves state-of-the-art and minimally invasive procedures to safely and effectively address your headache disorder. Call us today to schedule your consultation or know more about our cervicogenic headache treatment options.